10 คำถาม Tennis elbow
HIGHLIGHTS:
- เจ็บข้อศอกด้านข้าง เกิดได้จากหลายสาเหตุ เช่น Tennis Elbow คือ ภาวะเอ็นข้อศอกด้านข้างเสื่อม ผิวข้อกระดูกอ่อนเสียหาย หินปูนแคลเซียมเกาะเส้นเอ็น ซึ่งวินิจฉัยได้โดยการซักประวัติและตรวจร่างกายที่เหมาะสมโดยแพทย์ที่มีประสบการณ์
- Tennis elbow อาจหายได้เองโดยไม่ต้องรับการรักษา แต่หากอาการไม่ดีขึ้นและปล่อยทิ้งไว้นานเกินไป อาจส่งผลให้ข้อศอกมีการบาดเจ็บซ้ำซ้อนต่อเนื่อง จนเกิดภาวะข้อศอกเสื่อมก่อนวัยอันควรได้
- การรักษา Tennis elbow โดยการผ่าตัดอาจมีความจำเป็นสำหรับผู้ที่ไม่ตอบสนองต่อการรักษาแบบไม่ต้องผ่าตัด ซึ่งการผ่าตัดที่เป็นที่ยอมรับในปัจจุบันคือ การผ่าตัดผ่านกล้อง arthroscopic surgery
10 คำถามไขข้อข้องใจเกี่ยวกับภาวะ Tennis elbow
ตัวอย่างผู้ป่วย เจ็บข้อศอก Tennis elbow และการรักษา
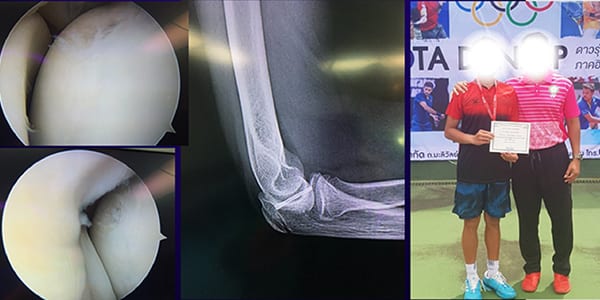
เด็กชายอายุ 14 ปี เป็นนักเทนนิส มาด้วยอาการเจ็บบริเวณเอ็นด้านข้างข้อศอก
โดยได้รับการรักษาแบบเทนนิสเอลโบ มาหลายเดือน อาการไม่ดีขึ้น แพทย์ผู้เขียนให้วินิจฉัยภาวะกระดูกอ่อนแตก เพราะข้อศอกมีการเคลื่อนไหวที่เสียหายและรักษาด้วยการหยุดเล่น ใส่กายอุปกรณ์ดามแล้วไม่หาย ซึ่งตรวจยืนยันแล้วว่ากระดูกอ่อนไม่ติดด้วยการ MRI ผู้ป่วยจึงได้รับการผ่าตัดผ่านกล้องยึดชิ้นกระดูกที่แตก ทำให้ผู้ป่วยสามารถกลับไปแข่งเทนนิสต่อได้
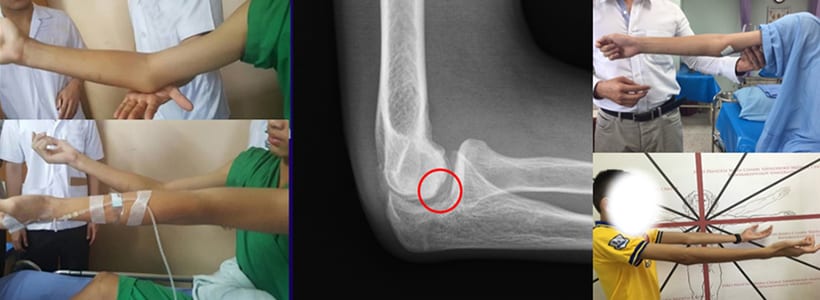
ชายอายุ 15 ปีเป็นนักเรียนกีฬายิมนาสติก มีอาการปวดเรื้อรังด้านข้างข้อศอกและข้อศอกเหยียดไม่สุด ได้รับการรักษาแบบ Tennis elbow
ด้วยการรับประทานยา กายภาพบำบัด พัก งดการซ้อม อาการก็ไม่ดีขึ้น จึงถูกส่งตัวมารักษา แพทย์ผู้เขียนให้การวินิจฉัยว่ากระดูกอ่อนผิวข้อแตกหลุด ผู้ป่วยได้รับการผ่าตัดผ่านกล้องแก้ไข หลังผ่าตัดผู้ป่วยสามารถเหยียดศอกได้ดีขึ้นอย่างชัดเจนใน1-2 วันหลังผ่าตัด
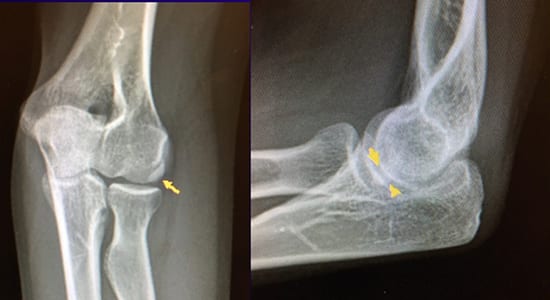
หญิงอายุ 26 ปี มีอาการเจ็บด้านข้างข้อศอกรุนแรงมากจนขยับข้อศอกได้น้อยลง ได้รับการการวินิจฉัยและรักษาแบบ tennis elbow
รักษาไม่หายจึงถูกส่งต่อมาให้แพทย์ผู้เขียน จากการตรวจร่างกายและส่งตรวจเพิ่มเติม ผู้ป่วยรายนี้ไม่เคยได้รับการตรวจเอกซเรย์ แพทย์ผู้เขียนจึงส่งไปตรวจและได้ให้การวินิจฉัยว่าเป็น ผลึกหินปูนเกาะเส้นเอ็น calcific tendinitis
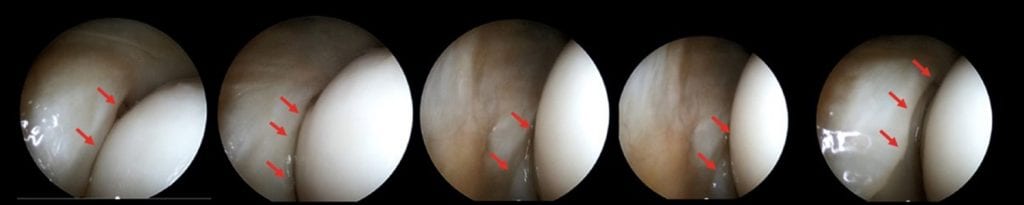
ชายอายุ 42 ปี มีอาชีพเป็นเจ้าของกิจการส่วนตัว เล่นกีฬา ออกกำลังกายที่ฟิตเนส เจ็บข้อศอก เป็นๆ หายๆ นาน 6 เดือน ได้รับวินิฉัยว่าเป็น tennis elbow
รักษาด้วยการรับประทานยา ฉีดยา พักการใช้งาน ทำกายภาพบำบัด และ Shock wave therapy (SWT) รวมถึงใช้ยาลดการอักเสบหลายชนิด แต่อาการไม่ดีขึ้น ผู้ป่วยถูกส่งตัวมาปรึกษากับแพทย์ผู้เขียน จากการส่องกล้องพบผังผืดขบเบียดในข้อเวลาข้อศอกเหยียดงอ ส่งผลให้เกิดการเจ็บเรื้องรัง ในผู้ป่วยรายนี้ได้รับการกรอตัดผังผืดผ่านกล้อง ก็สามารถแก้ปัญหาได้

หญิงอายุ 39-45 ปี ได้รับการวินิจฉัยว่าเป็นเทนนิสเอลโบ (Tennis elbow) และรักษาโดยการฉีดยาสเตียรอยด์ 3-5 ครั้ง ช่วงหลังอาการปวดรุนแรงมากขึ้น
ลักษณะอาการเปลี่ยนแปลงและระยะเวลาหายปวดหลังฉีดสเตียรอยด์สั้นมากกว่าเดิมมาก จากการผ่าตัดผ่านกล้อง พบว่า สาเหตุที่ทำให้เจ็บเรื้อรังคือผังผืดขบในข้อ ซึ่งสามารถรักษาโดยการกรอตัดออก แต่เนื่องจากผู้ป่วยรายนี้ ได้รับสเตียรอยด์ซ้ำๆ จนเส้นเอ็นหย่อนยาน ที่ดูได้จากภาพที่ข้อศอกหลวมออกมา จำเป็นต้องได้รับการผ่าตัดสร้างเส้นเอ็นเพิ่มเติม lateral collateral ligament reconstruction
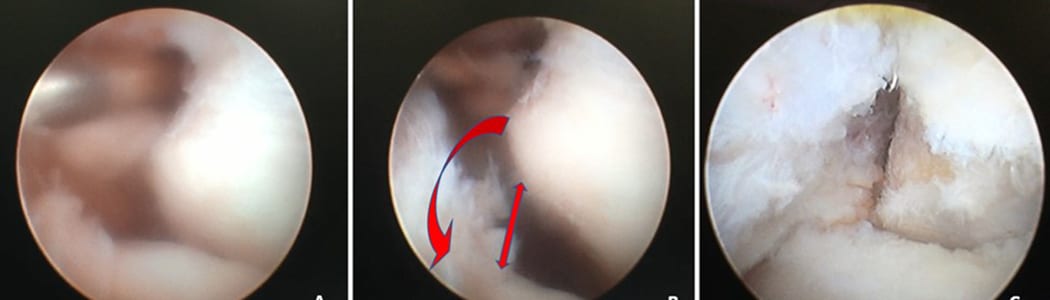
พยาบาล อายุ 42 ปี ไม่สามารถวิดพื้นหรือดันตัวจากเก้าอี้ได้ เพราะอาการปวดข้อศอก
รักษาด้วยการรับประทานยา กายภาพบำบัด และฉีดสเตียรอยด์มาแล้ว 3 ครั้ง แต่อาการไม่ดีขึ้น พบภาวะเอ็นข้อศอกหย่อนยานจากยาสเตียรอยด์ จึงจำเป็นต้องผ่าตัดสร้างเอ็นขึ้นมาแก้ปัญหา
